There’s a Special Enrollment Period Available if you Experienced Plan Finder Problems
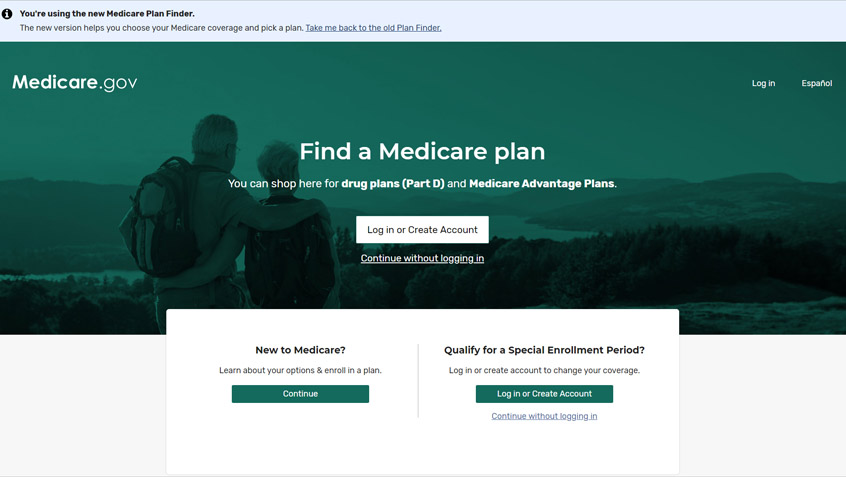
The Centers for Medicare & Medicaid Services (CMS) updated the Medicare Plan Finder this summer, providing much-needed changes to the look and feel and user experience of the federal government’s primary tool for looking up Medicare health and drug plans.
During Fall Open Enrollment—the time of year from October 15 to December 7 when people with Medicare can make unrestricted changes to their coverage—there were reports of Plan Finder sometimes displaying inaccurate or confusing information about drug costs and coverage. This may have led individuals to enroll in a plan that is not appropriate for their situation.
[x_custom_headline level=”h4″ looks_like=”h5″ accent=”false” style=”margin-top:0px;”]Advice for anyone who chose a plan using the new Plan Finder:[/x_custom_headline]
If you are dissatisfied with your plan selection because of misinformation you saw on Plan Finder, you can use a special circumstances Special Enrollment Period (SEP) to choose a new plan. This SEP exists to address enrollment problems that do not fit into any other SEP category or that are related to misinformation received from plans or Medicare.
To use this SEP:
- Call 1-800-MEDICARE (633-4227).
- Explain your situation to the customer service representative.
- Be prepared with the name of the new Medicare Advantage or stand-alone Part D plan you want to enroll in.
There is no deadline for making a new enrollment request, and you should not be required to provide proof of the misinformation or confusion you experienced. If you have any issues using this SEP when you call Medicare, ask to speak with a supervisor. You can also contact your State Health Insurance Assistance Program (SHIP) for help by visiting www.shiptacenter.org or calling 877-839-2675.
As a reminder, if you are unhappy with your plan choice because you received misleading marketing materials directly from a plan, you can also use an SEP to enroll in new coverage. Visit Medicare Interactive for more information.
Show Comments
The Latest
Most Read
Sorry. No data so far.
Add Medicare to Your Inbox
Sign up to receive Medicare news, policy developments, and other useful updates from the Medicare Rights.
View this profile on InstagramMedicare Rights Center (@medicarerights) • Instagram photos and videos





