Pfizer COVID-19 Vaccine Boosters Covered by Medicare with No Cost-Sharing
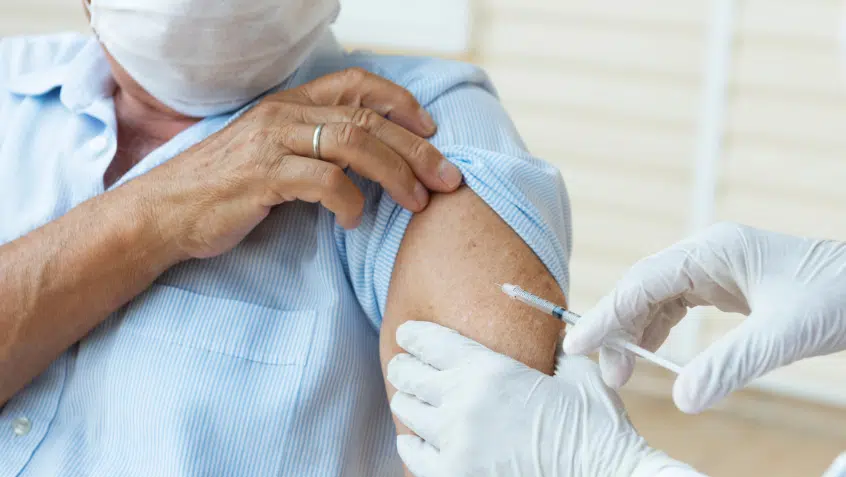
The Centers for Medicare & Medicaid Services (CMS) recently announced Medicare will cover booster doses of the Pfizer COVID-19 vaccine without any cost-sharing. As with the initial vaccinations, there will be no applicable copayment, coinsurance, or deductible.
Medicare beneficiaries who are 65 and older or at high risk can get the shot six months after they receive their second dose of the Pfizer COVID-19 vaccine. The Pfizer boosters are authorized by the Food and Drug Administration (FDA) and recommended by the Centers for Disease Control and Prevention (CDC). The agencies expect decisions about boosters for people who received the Moderna or Johnson & Johnson vaccines will be forthcoming.
CMS also said the boosters will be covered without cost-sharing for nearly all Medicaid and Children’s Health Insurance Program (CHIP) enrollees, and for eligible consumers in the commercial health insurance market.
This coverage policy comes at a critical time. As the CDC explained, “[w]ith the Delta variant’s dominance as the circulating strain and cases of COVID-19 increasing significantly across the United States, a booster shot will help strengthen protection against severe disease” for those who are vulnerable to exposure or serious illness.
Since the start of the pandemic, older adults have been among the hardest-hit populations, experiencing higher rates of hospitalization and death than other age groups. While these instances declined once widespread vaccination efforts began, a new Kaiser Family Foundation (KFF) analysis reveals a troubling trend: COVID-19 related deaths among older adults are on the rise amid the Delta surge.
One reason for this could be lagging vaccinations. Recent CDC data show vaccines remain effective at preventing hospitalizations and death. Although older adults have the highest vaccination rate among all age groups (83.7%), it varies widely across states, from 95.3% in Vermont to just 71.3% in West Virginia.
The KFF report indicates there is a correlation. The authors found that during the study period (July 1 through September 25), states with the lowest vaccination rates had the highest death rates, at nearly two times the national average of 93 per 100,000 people 65 and older. Conversely, states with the highest vaccination rates experienced relatively low death rates. For example, in Massachusetts, 88.8% of older adults have been vaccinated and the death rate (28 per 100,000) was about 7 times lower than in Arkansas (198 per 100,000), which has a vaccination rate of 72.8%.
KFF notes other factors could also be at work—many older adults were among the first to receive the COVID-19 vaccine and may be among the first to experience decreasing vaccine effectiveness over time—which the booster shots could help address.
Read more from CMS about Medicare coverage of COVID-19 vaccines.
To search for vaccines near you, visit vaccines.gov (English) or vacunas.gov (Spanish).
Show Comments
The Latest
Most Read
Sorry. No data so far.
Add Medicare to Your Inbox
Sign up to receive Medicare news, policy developments, and other useful updates from the Medicare Rights.
View this profile on InstagramMedicare Rights Center (@medicarerights) • Instagram photos and videos





